-
Active monitoring
Active monitoring, also known as watch and wait, is a method of managing a blood cancer or blood condition over a period of time without receiving treatment right away.

-
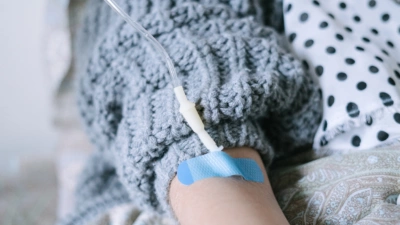
Chemotherapy
Generally, chemotherapy drugs are the main form of treatment for cancer. There are many different types of chemotherapy drugs, and each drug affects the cancer cells in different ways.
-
Corticosteroid therapy (steroids)
Corticosteroids (often just called steroids) are drugs that mimic different hormones in the body.

-
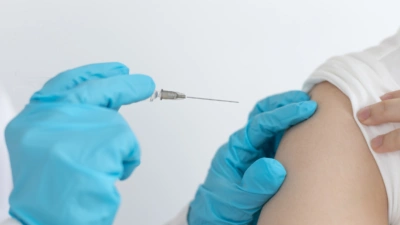
Immunotherapy
Immunotherapy is the use of drugs to help a person’s own immune system recognise and destroy cancer cells.
-
Palliative care
Palliative care is aimed at relieving any symptoms or pain you may be experiencing as a result of your blood cancer or its treatment, rather than trying to cure or control it.

-
Radiotherapy
Radiotherapy (also called radiation therapy) is a type of treatment that uses high energy x-rays to kill cancer cells and shrink tumours.

-
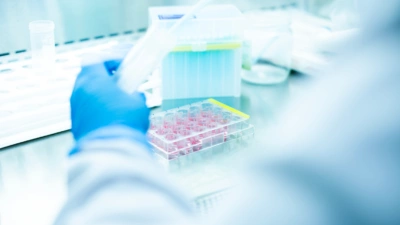
Stem cell transplant
A stem cell transplant is a treatment option for some people who have a blood cancer or blood condition.
-
Supportive care
Supportive care aims to improve the quality of life of people who have a blood cancer or blood condition.

-
Targeted therapy
Targeted therapies are a group of drugs that block the growth and spread of cancer cells by interfering with specific molecules.

-
Common side effects of treatment
The type of side effects and their severity varies from person to person, depending on the type of treatment used and how an individual responds to it.

-
Accessing Unfunded Treatments
This information is intended as a guide for those seeking access to treatments not funded by Pharmac. Your first step is always to discuss with your haematologist whether you are likely to benefit from an unfunded treatment. They can provide guidance on the need for a specific medication and prescribe, as required.

-
Accessing Treatment Overseas
Medicine availability in New Zealand is limited compared to other countries such as Australia and the UK. This is in part due to differences in how our medicine buying agency, Pharmac, operates.

- 1
- 2